AbstractA survey of intestinal helminths was undertaken in riparian people in Xieng Khouang Province, Lao PDR. Fecal specimens were collected from 643 people (289 males and 354 females) residing in 4 districts (Nonghet, Kham, Phoukout, and Pek) and were examined by the Kato-Katz technique. The overall helminth egg positive rate was 41.2%, and hookworms revealed the highest prevalence (32.7%) followed by Trichuris trichiura (7.3%) and Ascaris lumbricoides (5.6%). The positive rate for small trematode eggs (STE), which may include Opisthorchis viverrini, heterophyids, and lecithodendriids, was 4.4%. For recovery of adult helminths, 12 STE or nematode/cestode egg-positive people were treated with 40 mg/kg praziquantel and 15 mg/kg pyrantel pamoate, and then purged. Mixed infections with 2 Haplorchis species (H. pumilio and H. taichui), Centrocestus formosanus, Opisthorchis viverrini, a species of cestode (Taenia saginata), and several species of nematodes including hookworms and Enterobius vermicularis were detected. The worm load for trematodes was the highest for H. pumilio with an average of 283.5 specimens per infected person followed by C. formosanus, H. taichui, and O. viverrini. The worm load for nematodes was the highest for hookworms (21.5/infected case) followed by E. vermicularis (3.2/infected case). The results revealed that the surveyed areas of Xieng Khouang Province, Lao PDR are endemic areas of various species of intestinal helminths. The STE found in the surveyed population were verified to be those of heterophyids, particularly H. pumilio.
INTRODUCTIONIn Lao People’s Democratic Republic (Lao PDR), various kinds of trematode infections have been prevalent among riparian people almost all over the country [1-6]. The liver fluke, Opisthorchis viverrini, is prevalent along the Mekong River, particularly in Vientiane, Khammouane, Savannakhet, and Champasak Provinces [2,4,7-11]. Mixed infections with O. viverrini and minute intestinal flukes including Haplorchis spp. (H. taichui, H. pumilio, and H. yokogawai) and lecithodendriids (Prosthodendrium molenkampi and Phaneropsolus bonnei) have also been reported in Vientiane Municipality and Saravane [2], Khammouane [9], and Savannakhet Provinces [8]. In contrast, northern mountainous areas including Phongsaly and Luang Prabang Province were infected exclusively with intestinal flukes H. taichui, H. yokogawai, and/or H. pumilio [3,6]. Centrocestus formosanus is another minute intestinal fluke species recovered recently from a few Laotians in scattered localities [12]. Schistosomiasis [13], paragonimiasis [14], and echinostomiasis [15,16] have also been reported from scattered localities in Lao PDR.
Xieng Khouang Province is located in a northeastern mountainous area of Lao PDR, and thus it is expected to have minute intestinal fluke infections, in particular, Haplorchis spp., just like Phongsaly and Luang Prabang Provinces [3,6]. However, according to the report by Rim et al. [1], Xieng Khouang Province was free from the eggs of O. viverrini or minute intestinal flukes, but highly prevalent with soil-transmitted helminths including Ascaris lumbricoides, hookworms, and Trichuris trichiura. The paucity of trematode infections in this area needs to be verified.
We surveyed for intestinal helminth infections among riparian people in 4 districts of Xieng Khouang Province, during the Korea-Laos International Collaboration Project entitled ‘Control of foodborne trematode infections among the Laotians (2007-2011)’ between the Korea Foundation for International Healthcare and Ministry of Public Health, Lao PDR. The aim of this study was to clarify the species of helminths infecting riparian people in Xieng Khouang Province, Lao PDR.
MATERIALS AND METHODSSurveyed areas and sample collectionThe surveyed areas consisted of 14 small riparian villages in 4 districts (Nonghet, Kham, Phoukout, and Pek) of Xieng Khouang Province, Lao PDR (Fig. 1). The river ‘Nam Khan’ runs through Nonghet and Kham Districts, and the river ‘Nam Ngum’ flows through Phoukout and Pek Districts. The whole population of Xieng Khouang Province was 229,521 as of 2005, and the population in the 4 districts was estimated to be about 120,000. Most residents were farmers and some were fishermen. In July 2011, a total of 643 fecal samples were collected from the residents (289 males and 354 females, 14-90 years of age, 1 sample per person). The fecal samples were transported to the Malaria Center, Provincial Health Department of Xienkhouang Province located in Phonsavan City. The Kato-Katz thick smear technique was applied for detection of helminth eggs (Table 1). Small trematode eggs (STE) denote small operculate eggs of 20-35 µm in length, which may include eggs of O. viverrini, heterophyids, and lecithodendriids.
Recovery of adult flukesTwelve STE and/or nematode/cestode egg-positive cases from Kham and Pek Districts, 29-63-year of age (11 men and 1 woman), who complained of indigestion and vague abdominal discomfort and agreed to receive this procedure were selected for anthelmintic treatment and purging to recover the adult worms (Table 2). This study followed the ethical guidelines of the Seoul National University College of Medicine, Seoul, Korea. Informed consent was obtained from each person. The patients were treated with a single oral dose of 40 mg/kg praziquantel (Shinpoong Pharm, Seoul, Korea) combined with 15 mg/kg pyrantel pamoate (Hangzhou Minseng Pharm, Hangzhou, China), and purged with 30-40 g MgSO4. Whole consecutive diarrheic stools were collected 3-5 times over 4-5 hr duration following purging. The diarrheic stools were pooled individually and processed as previously described [4,6,9]. The collected helminth specimens were fixed in 10% formalin or 70% ethanol, stained with Semichon’s acetocarmine, and morphologically identified. Fecal examination and anthelmintic treatment of the patients were approved by the Ministry of Public Health, Lao PDR, under the agreement of the Korea-Laos International Collaboration (2007-2011).
RESULTSPrevalence of helminth eggsAmong the 643 fecal samples examined, the egg positive rate slightly varied by the village (32.6-48.8%) with an average egg positive rate of 41.2% (Table 1). Differences in the prevalence between men and women were not statistically significant (data not shown, P>0.05). The highest prevalence was found in Nonghet District (48.8%) followed by Kham (46.1%), Phoukout (34.3%), and Pek Districts (32.6%). The most commonly encountered helminth eggs were those of soil-transmitted nematodes including hookworms (32.7%), T. trichiura (7.3%), and A. lumbricoides (5.6%), which was followed by eggs of foodborne helminths including STE (4.4%), Taenia spp. (1.6%), and echinostomes (0.6%) (Table 1). The prevalence of hookworms varied from 20.4% (Phoukout) and 27.9% (Pek) to 39.3% (Kham) (difference between Kham and the 2 other districts, P<0.05). T. trichiura was more prevalent in Kham (16.2%) than in the three other districts (1.9-5.2%) (P<0.05). The prevalence of A. lumbricoides was in the range of 1.7-9.3%.
Regarding STE, the prevalence varied slightly by the district, the highest in Phoukout (7.4%) followed by Kham (4.7%), Nonghet (3.5%), and Pek Districts (2.9%) (Table 1). The prevalence of Taenia spp. was not significantly different by the district, remaining in the range of 0.6-2.8% (P>0.05).
Recovery of helminth specimens from 12 patientsA total of 2,686 helminth specimens (2,487 trematodes, 191 nematodes, and 8 cestodes) were collected from the diarrheic stool of 12 patients (A-L) after anthelmintic treatment and purging (Table 2). They comprised 8 species, including 2 Haplorchis spp., C. formosanus (reported previously by Chai et al. [12]), O. viverrini, Taenia saginata (reported previously by Jeon et al. [17]), and 3 species of nematodes (2 hookworm species and E. vermicularis). Hookworm species consisted of Ancylostoma duodenale and Necator americanus at an approximate ratio of 6:4. Trematodes were predominantly composed of Haplorchis spp., with the great majority being H. pumilio (91.2%; 2,268/2,487 specimens) (Fig. 2) and a few being H. taichui (3.7%; 93/2,487 specimens), C. formosanus (4.9%; 122/2,487 specimens), and O. viverrini (0.2%; 4/2,487 specimens). Lecithodendriids were not recovered. Eight Taenia saginata specimens were recovered from 7 patients (Table 2). Among the 191 nematode specimens, 172 (90.1%) were hookworms (in 82 males and 90 females), which were recovered from 8 out of the 12 patients (21.5 specimens per positive person). Nineteen specimens (9.9%), 5 males and 14 females, of E. vermicularis were recovered from 6 out of the 12 patients.
The heaviest worm load for H. pumilio was 1,542 specimens in patient A. In this patient, the eggs per gram of feces (EPG) for STE measured on a Kato-Katz smear was 432 (Table 2). The second heaviest worm load was seen in patient B (403 specimens, EPG 48). From 6 other patients, 1-158 H. pumilio specimens were recovered. The average worm load for H. pumilio from these 8 patients was 283.5. H. taichui was recovered from only 1 patient (93 specimens). Three out of these 8 patients were negative for STE in Kato-Katz smears but after treatment and purging 1-39 specimens of H. pumilio were collected (Table 2).
DISCUSSIONIn northern mountainous areas of Lao PDR, including Phongsaly and Luang Prabang Provinces, Haplorchis spp. but not O. viverrini were reported to be prevalent among riparian people [3,6]. A similar pattern was found in Xieng Khouang Province in this study. The most common species was H. pumilio which was detected in 8 out of the 12 treated-purged patients. O. viverrini worms were recovered from 2 out of the 12 patients, and C. formosanus and H. taichui were detected in 1 patient each.
The recovery of 4 O. viverrini specimens from 2 patients was noteworthy, because the life cycle of O. viverrini may be present in this area. However, it was stated by the local people that some freshwater fish are imported to Xieng Khouang Province from Vientiane Municipality where O. viverrini is endemic [2]. The 2 patients might have consumed O. viverrini-infected fish from Vientiane Municipality. However, this cannot be verified and we cannot completely rule out the possibility of a low-grade endemicity of O. viverrini in Xieng Khouang Province. This issue needs to be assessed further.
The predominance of H. pumilio over H. taichui or H. yokogawai in this area is interesting. In Phongsaly Province, located far northwest of Xieng Khouang Province, none of the patients were infected with H. pumilio, whereas 6-8 out of the 10 patients treated and purged expelled substantial numbers of H. taichui and H. yokogawai worms after treatment [3]. In Luang Prabang Province, a neighbor province located northwest of Xieng Khouang Province, all 3 Haplorchis spp. were recovered with H. taichui being the most common species [6]. In other provinces of Lao PDR, including Vientiane, Savannakhet, Khammouane, Saravane, and Champasak Provinces, H. taichui was always the most prevalent intestinal fluke species compared with H. pumilio and H. yokogawai [2,4,8,9]. On the contrary, in Nam Dinh Province of Vietnam, a neighbor country, east to Xieng Khouang Province, the predominance of H. pumilio over H. taichui and H. yokogawai was reported previously [18]. The Nam Dinh Province of Vietnam and Xieng Khouang Province of Lao PDR are very close and just facing each other; thus, the distribution of intestinal flukes may be similar. However, this possible trend also needs to be verified further.
The symptoms in our patients including indigestion and vague abdominal discomforts may not necessarily be due to Haplorchis spp. infection, since there were mixed-infections with other helminths including Taenia tapeworms, hookworms, and pinworms. It is generally accepted that minute intestinal flukes are less pathogenic than liver or lung flukes [19]. However, several recent reports described pathogenicity of Haplorchis flukes in humans. In 3 patients heavily infected with H. taichui in northern Thailand, the small intestinal mucosa revealed ulceration, hemorrhage, fusion and shortening of villi, chronic inflammation, and fibrosis of the submucosa, which clearly implicated that H. taichui is pathogenic [20]. In another area of Thailand, where villagers were infected only with H. taichui but not with other intestinal fluke species or O. viverrini, more than a half of the infected people complained of abdominal pain, lassitude, and flatulence, which were consistent with irritable bowel syndrome [21].
Abiding to intestinal fluke infections, particular attention should be paid to hookworm infections in the surveyed population. The average prevalence was 32.7% (210/643) and the worm load was fairly high (average 21.5 worms per infected person). This prevalence was similar to that (37.7%) in our previous study [1] and that (39.5%) in another study in Xieng Khouang Province [22]. However, the rate was somewhat higher than the average nationwide figure (19.1-27.8%) in Lao PDR [1,23]. The worm load was much higher compared to that in other areas including Luang Prabang [6] and Phongsaly Province [3].
Regarding Taenia tapeworm infections, several studies have been performed in Lao PDR [17,24,25]. The overall egg positive rate of Taenia spp. among 55,038 Laotians from different parts of the country (2002-2011) was 1.5% [17]. As to the species of Taenia, 123 of 126 adult specimens recovered from patients after praziquantel treatment and purging were confirmed to be Taenia saginata by molecular studies, while the remaining 3 were Taenia solium but none were Taenia asiatica [17]. On the other hand, the prevalence of taeniases was as high as 8.4% among people in 4 northern provinces (Oudomxay, Luangprabang, Huaphan, and Xieng Khouang) [25]. In our study, the prevalence of Taenia spp. eggs was 1.6%, similar to the general figure in Lao PDR [17]. The species in this area was molecularly confirmed to be T. saginata [17].
Taken together, the results of the present study suggest that there is an urgent need to control intestinal fluke as well as intestinal nematode and cestode infections in the surveyed areas of Xieng Khouang Province, Lao PDR. The STE found in this area appeared to be predominantly those of Haplorchis spp., in particular, H. pumilio.
ACKNOWLEDGEMENTSWe are grateful to the staff of Malaria Center, Provincial Health Department, Xieng Khouang Province, Lao PDR for their assistance in collecting fecal specimens and preparing the Kato-Katz thick smears.
Conflict of interestThe authors declare that they have no conflict of interest related to this study.
REFERENCES1. Rim HJ, Chai JY, Min DY, Cho SY, Eom KS, Hong SJ, Sohn WM, Yong TS, Deodato G, Standgaard H, Phommasack B, Yun CH, Hoang EH. Prevalence of intestinal parasite infections on a national scale among primary schoolchildren in Laos. Parasitol Res 2003;91:267-272.
2. Chai JY, Park JH, Han ET, Guk SM, Shin EH, Lin A, Kim JL, Sohn WM, Yong TS, Eom KS, Min DY, Hwang EH, Phommasack B, Insisiengmai B, Rim HJ. Mixed infections with Opisthorchis viverrini and intestinal flukes in residents of Vientiane Municipality and Saravane Province in Laos. J Helminthol 2005;79:283-289.
3. Chai JY, Yong TS, Eom KS, Min DY, Shin EH, Banouvong V, Insisiengmay B, Insisiengmay S, Phommasack B, Rim HJ. Prevalence of the intestinal flukes Haplorchis taichui and H. yokogawai in a mountainous area of Phongsaly Province, Lao PDR. Korean J Parasitol 2010;48:339-342.
4. Chai JY, Yong TS, Eom KS, Min DY, Jeon HK, Kim TY, Jung BK, Sisabath L, Insisiengmay B, Phommasack B, Rim HJ. Hyperendemicity of Haplorchis taichui infection among riparian people in Saravane and Champasak Province, Lao PDR. Korean J Parasitol 2013;51:305-311.
5. Sayasone S, Vonghajack Y, Vanmany M, Rasphone O, Tesana S, Utzinger J, Akkhavong K, Odermatt P. Diversity of human intestinal helminthiasis in Lao PDR. Trans R Soc Trop Med Hyg 2009;103:247-254.
6. Sohn WM, Yong TS, Eom KS, Min DY, Lee D, Jung BK, Banouvong V, Insisiengmay B, Phammasack B, Rim HJ, Chai JY. Prevalence of Haplorchis taichui among humans and fish in Luang Prabang Province, Lao PDR. Acta Trop 2014;136:74-80.
7. Chai JY, Hongvanthong B. A small-scale survey of intestinal helminthic infections among the residents near Pakse, Laos. Korean J Parasitol 1998;36:55-58.
8. Chai JY, Han ET, Guk SM, Shin EH, Sohn WM, Yong TS, Eom KS, Lee KH, Jeong HG, Ryang YS, Hoang EH, Phommasack B, Insisiengmai B, Lee SH, Rim HJ. High prevalence of liver and intestinal fluke infections among residents of Savannakhet Province, Laos. Korean J Parasitol 2007;45:213-218.
9. Chai JY, Han ET, Shin EH, Sohn WM, Yong TS, Eom KS, Min DY, Um JY, Park MS, Hoang EH, Phommasack B, Insisiengmay B, Lee SH, Rim HJ. High prevalence of Haplorchis taichui, Prosthodendrium molenkampi, and other helminth infections among people in Khammouane Province, Lao PDR. Korean J Parasitol 2009;47:243-247.
10. Sayasone S, Mak TK, Vanmany M, Rasphone O, Vounatsou R, Utzinger J, Akkhavong K, Odermatt P. Helminth and intestinal protozoa infections, multiparasitism and risk factors in Champasack Province, Lao PDR. PLoS Negl Trop Dis 2011;5:e1037.
11. Sato M, Pongvongsa T, Sanguankiat S, Yoonuan T, Kobayashi J, Boupha B, Nishimoto F, Moji K, Sato MD, Waikagul J. Patterns of trematode infections of Opisthorchis viverrini (Opisthorchiidae) and Haplorchis taichui (Heterophyidae) in human populations from two villages in Savannakhet Province, Lao PDR. J Helminthol 2015;89:439-445.
12. Chai JY, Sohn WM, Yong TS, Eom KS, Min DY, Lee MY, Lim H, Insisiengmay B, Phammasack B, Rim HJ. Centrocestus formosanus (Heterophyidae): human infections and the infection source in Lao PDR. J Parasitol 2013;99:531-536.
13. Muth S, Sayasone S, Odermatt-Biays S, Phomphida S, Duong S, Odermatt P. Schistosoma mekongi in Cambodia and Lao Peoples’ Democratic Republic. Adv Parasitol 2010;72:179-203.
14. Odermatt P, Veasna D, Zhang W, Vannavong N, Phrommala S, Habe S, Barennes H, Strobel M. Rapid identification of paragonimiasis foci by lay informants in Lao Peoples’ Democratic Republic. PLoS Negl Trop Dis 2009;3:e521.
15. Sayasone S, Tesana S, Utzinger J, Hatz C, Akkhavong K, Odermatt P. (2009b) Rare human infection with the trematode Echinochasmus japonicus in Lao PDR. Parasitol Int 2009;58:106-109.
16. Chai JY, Sohn WM, Yong TS, Eom KS, Min DY, Hoang EH, Phammasack B, Insisiengmay B, Rim HJ. Echinostome flukes recovered from humans in Khammouane Province, Lao PDR. Korean J Parasitol 2012;50:269-272.
17. Jeon HK, Yong TS, Sohn WM, Chai JY, Min DY, Yun CH, Rim HJ, Pongvongsa T, Banouvong V, Insisiengmay B, Phommasack B, Eom KS. Current status of human taeniasis in Lao People’s Democratic Republic. Korean J Parasitol 2013;51:259-263.
18. Dung DT, De NV, Waikagul J, Dalsgaard A, Chai JY, Sohn WM, Murrell KD. Fishborne zoonotic intestinal trematodes, Vietnam. Emerg Infect Dis 2007;13:1828-1833.
19. Chai JY, Murrell KD, Lymbery AJ. Fish-borne parasitic zoonoses: status and issues. Int J Parasitol 2005;35:1233-1254.
20. Sukontason K, Unpunyo P, Sukontason KL, Piangjai S. Evidence of Haplorchis taichui infection as pathogenic parasite: three case reports. Scand J Infect Dis 2005;37:388-390.
21. Watthanakulpanich D, Waikagul J, Maipanich W, Nuamtanong S, Sanguankiat S, Pubampen S, Praevanit R, Mongkhonmu S, Nawa Y. Haplorchis taichui as a possible etiologic agent of irritable bowel syndrome-like symptoms. Korean J Parasitol 2010;48:225-229.
22. Laymanivong S, Hongvanthong B, Phommasack M, Phinmaland B, Sanpool O, Maleewong W, Intapan PM. Current status of human hookworm infections, ascariasis, trichuriasis, schistosomiasis mekongi and other trematodiases in Lao Peoples’ Democratic Republic. Am J Tryp Med Hyg 2014;90:667-669.
23. Eom KS, Yong TS, Sohn WM, Chai JY, Min DY, Rim JH, Jeon HK, Banouvong V, Insisiengmay B, Phommasack B. Prevalence of helminthic infections among inhabitants of Lao PDR. Korean J Parasitol 2014;52:51-56.
Fig. 1.Map showing the surveyed areas of Xieng Khouang Province, Lao PDR. Fourteen riparian villages (small circles) located in 4 districts (Nonghet, Kham, Phoukout, and Pek) were included in this study. 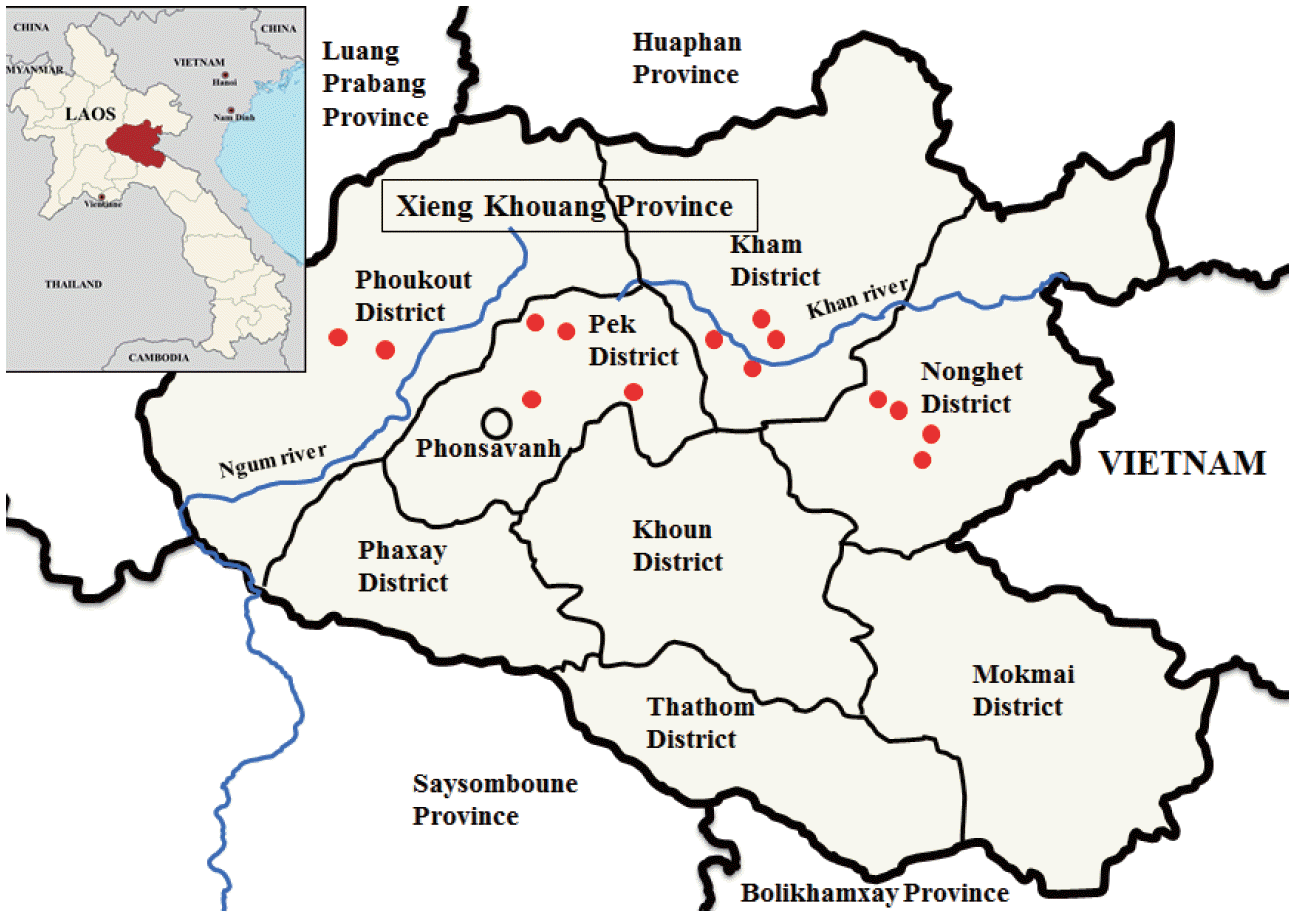
Fig. 2.An adult specimen (A, B) of H. pumilio. (A) The adult fluke (0.62 mm long) was recovered from a patient in Kham District after chemotherapy and purging. The gonotyl (arrows) is seen on the right side of the worm. Scale bar=0.07 mm. (B) A close-up view of the gonotyl and gonotyl spines (arrows). About 40 small chitinous spines are seen on this worm. Scale bar=0.04 mm. 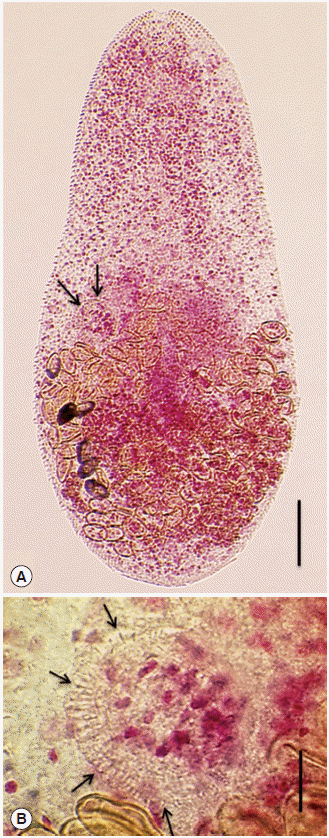
Table 1.Prevalence of intestinal helminths among people in Xieng Khouang Province, Lao PDR
Table 2.Worm recovery from 12 helminth egg positive cases in Kham and Pek Districts, Xieng Khouang Province, Lao PDR
|
|
|||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||