INTRODUCTION
Detection of eggs in stool can lead to a definite diagnosis of Clonorchis sinensis infection (clonorchiasis), thus, clonorchiasis has been principally diagnosed by stool microscopic examination. There are several methods of stool microscopic examination, but the Kato-Katz method is regarded as the best one for clonorchiasis (Hong et al., 2003). However, the routine stool microscopic examinations usually performed in hospitals (without a specialized laboratory for parasites) are insufficient to detect a few C. sinensis eggs in the stool of patients with a light infection. Furthermore, collection of stools is becoming rather difficult due to low compliance of residents. In this context, several other diagnostic tools such as skin tests, serologic tests and radiologic examinations have been introduced. The skin test is known to be sensitive but not specific, and enzyme-linked immunosorbent assay (ELISA) is widely used for serodiagnosis with moderate sensitivity and specificity but cross reactions occur with other parasitic fluke infections (Chen et al., 1994; Hong, 2003).
As a majority of physicians have little interest and knowledge in clonorchiasis, neither of stool examination, skin test, and ELISA for clonorchiasis is recommended as a routine examination for patients with vague epigastric pain or non-specific symptoms of the digestive tract even in endemic areas. Practically, clonorchiasis is commonly diagnosed during sonographic examination of the abdomen mainly for other purposes.
At present, clonorchiasis is still endemic along several rivers and about 1.3 million infected people are estimated over the country in Korea (KAHP, 2004). It must be one major health problem in endemic areas, which should be of priority. The health authority and local governments in endemic areas are trying to find out infected residents and to treat them with praziquantel, but their trials are not so effective because its diagnosis is rather difficult.
In the present article, we reviewed imaging findings of clonorchiasis, including cholangiography, sonography, computed tomography (CT), and magnetic resonance (MR) imaging. We tried to summarize imaging findings and suggest guidelines for imaging diagnosis of clonorchiasis.
CHOLANGIOGRAPHIC FINDINGS OF CLONORCHIASIS
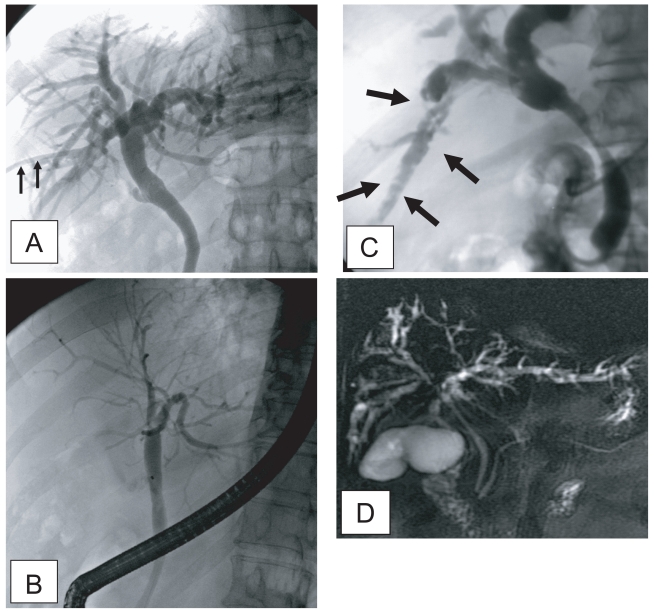
The principle imaging finding of clonorchiasis is diffuse dilatation of the peripheral intrahepatic bile ducts (Lim, 1990). However, the larger intrahepatic and extrahepatic bile ducts are not dilated or minimally dilated. The predominant dilatation of the peripheral intrahepatic ducts is due to the adult worms residing in the peripheral small bile ducts. Compared with normal subjects, many intrahepatic bile ducts are observed on cholangiography in patients with clonorchiasis due to the dilated peripheral intrahepatic bile ducts (Fig. 1A and B). Lim et al. (1992) reported "too many intrahepatic ducts" sign in 76% (22 of 29) of patients with clonorchiasis on direct cholangiography.
The presence of the fluke bodies in the peripheral bile ducts can be demonstrated on a cholangiogram (Choi et al., 1984; Lim et al., 1992). Cholangiography shows oval, elliptical, or filamentous, small filling defects within the dilated peripheral intrahepatic bile ducts, representing the flukes (Fig. 1) (Lim et al., 1992). It is a pathognomonic finding on direct cholangiography, but the defects can be obscured by the contrast medium. The filling defects by the flukes are usually small and irregular, with a uniform size on direct cholangiography, which are easily differentiated from stones (Fig. 1) (Choi et al., 1984; Lim et al., 1992; Jeong et al., 2004). Direct cholangiogram is obtained with an injection of iodine contrast material via catheter during either endoscopy or percutaneous biliary drainage (Fig. 1). Recently, non-invasive cholangiograms can be made by using MR imaging (Fig. 1) (Barish and Soto, 1997).
SONOGRAPHIC FINDINGS OF CLONORCHIASIS
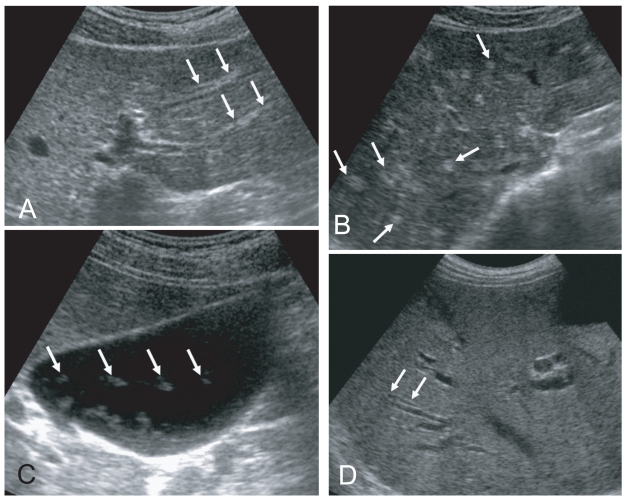
Sonographic findings of diffuse dilatation of the intrahepatic bile ducts and increased periductal echogenicity are known to well reflect pathological changes associated with clonorchiasis (Fig. 2) (Lim et al., 1989; Hong et al., 1994). Sonography is considered a good tool for the diagnosis of clonorchiasis, particularly in cases with a moderate or heavy burden of worms. According to a prior study in Korea, sonography showed low sensitivity and low specificity in the diagnosis of active clonorchiasis (Hong et al., 1998). The study suggested that the low sensitivity was due to a light worm burden and that the low specificity was due to residual pathology after cure.
In a recent study conducted by us in China, increased periductal echogenicity and floating echogenic foci in the gallbladder were proposed as the 2 most significant sonographic findings of active clonorchiasis (Choi et al., 2004). Increased periductal echogenicity represents a thickening of the ductal wall according to mucosal hyperplasia and periductal fibrosis, and the floating echogenic foci indicate worms or desquamated material in the gallbladder (Figs. 2A, B, C) (Lim et al., 1989; Hong et al., 1994; Choi et al., 1999). In our study in China, increased periductal echogenicity showed a sensitivity and specificity for active clonorchiasis of 35% and 91%, respectively (Choi et al., 2004). Floating echogenic foci in the gallbladder had a sensitivity and specificity of 28% and 94%, respectively. However, floating echogenic foci within the gallbladder have been rarely documented in Korea (Lim et al., 1989; Lim, 1990).
In the past literature, diffuse dilatation of the intrahepatic bile ducts on sonographic examination has been considered a hallmark of clonorchiasis (Lim et al., 1989; Lim, 1990; Hong et al., 1994). Diffuse dilatation of the intrahepatic bile ducts was found in an about half (49-52%) of the control subjects in either present endemic area or past endemic area (Fig. 2D) (Hong et al., 1998; Choi et al., 2004). Thus, patients only with a dilatation of the intrahepatic bile ducts detected by sonography cannot be considered candidates for praziquantel treatment (Chen et al., 1994; Hong et al., 1998; Choi et al., 1999). In an experimental study, the histopathological specimens at 18 mo after treatment with praziquantel showed that periductal inflammation has almost resolved but moderate dilatation of the intrahepatic ducts and mucosal hyperplasia persisted (Choi et al., 1999). The periductal fibrosis minimally resolved.
Although sonography is used as one of the screening diagnostic tools for clonorchiasis in endemic areas, sonography is a basically operator-dependent modality. Unless specific information is offered, many physicians and even radiologists cannot aware subtle changes of the intrahepatic bile ducts. It leads to low sensitivity to diagnose clonorchiasis, particularly in patients with light infection. Practically it is very difficult to make a correct diagnosis of lightly infected clonorchiasis by any method, even by stool examination (Hong et al., 2003). Choi et al. (2005) recorded a significant correlation of the sonographic findings with egg counts. The correlation was significant by both frequency and grade of the findings. In other words, the more the flukes were, the more and severer were the findings.
CT FINDINGS OF CLONORCHIASIS
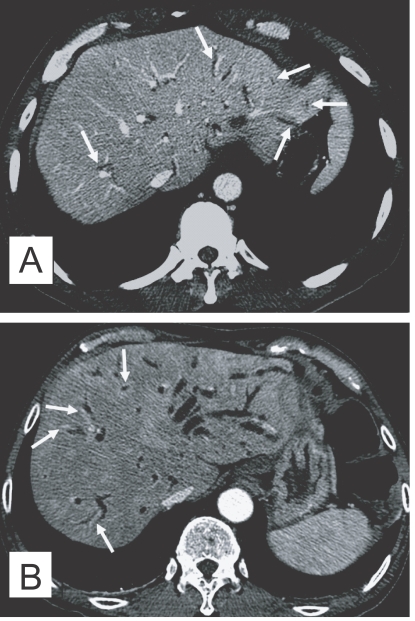
The CT finding of clonorchiasis is diffuse dilatation of the peripheral intrahepatic bile ducts, without dilation of the larger bile ducts or extrahepatic ducts (Fig. 3A). This finding is known to be the pathognomonic findings of clonorchiasis (Lim, 1990), however, it is also observed in cured infection.
In contrast to sonography showing an increased echogenicity of the ductal wall, CT failed to show thickening of the bile duct wall (Choi et al., 1989). A recent experimental study, however, suggested that an active infection could be differentiated from cured clonorchiasis by using the periductal enhancement with the thickened bile duct walls on dynamic contrast-enhanced CT (Lee et al., 2003). The contrast-enhanced CT visualized a characteristic finding, transient hepatic attenuation differences (THAD). The finding was interpreted as an outcome of new vascularization in the thickened bile duct wall, which disappeared after cure of clonorchiasis (Fig. 3B). They also asserted that some adult worms were demonstrated on their thin-section CT scans (Lee et al., 2003).
MR IMAGING FINDINGS OF CLONORCHIASIS
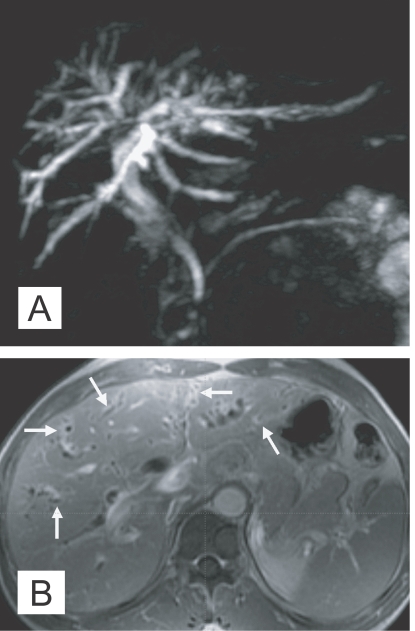
MR imaging has been used in diagnosis of various diseases of the biliary system, and MR cholangiography is a relatively new non-invasive imaging modality for evaluation of the biliary pathology. MR imaging can show the characteristic findings of clonorchiasis with diffuse, mild dilation of the small intrahepatic bile ducts, particularly in the periphery of the liver (Choi et al., 1998). According to a recent study, MR cholangiography also found "too many intrahepatic ducts" sign in 62% (16 of 26) of patients with clonorchiasis (Jeong et al., 2004). Periductal enhancement was more frequently seen on MR imaging, compared to CT, due to a higher spatial resolution of the soft tissue (Fig. 4). The filling defects representing worms were elliptical, irregular shaped, and hypointense lesions on the T2-weighted images and MR cholangiography.
IMAGING FINDINGS OF CHOLANGIOCARCINOMA ASSOCIATED WITH CLONORCHIASIS
The International Agency for Research on Cancer working group (1994) suggested that C. sinensis is a presumed carcinogen. Now, the relationship between clonorchiasis and cholangiocarcinomas is generally accepted, as epidemiological, pathological and experimental evidences, indicating a positive correlation, have been accumulated (Belamaric, 1973; Shin et al., 1996; Lee et al., 1997; Choi et al., 2006; Lim et al., 2006).
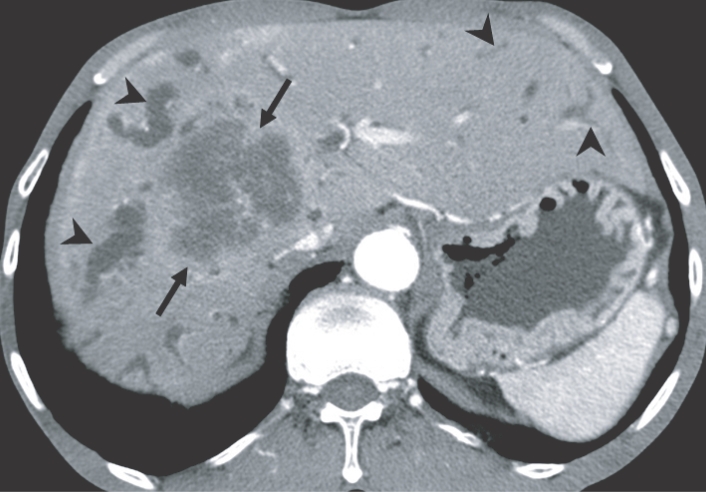
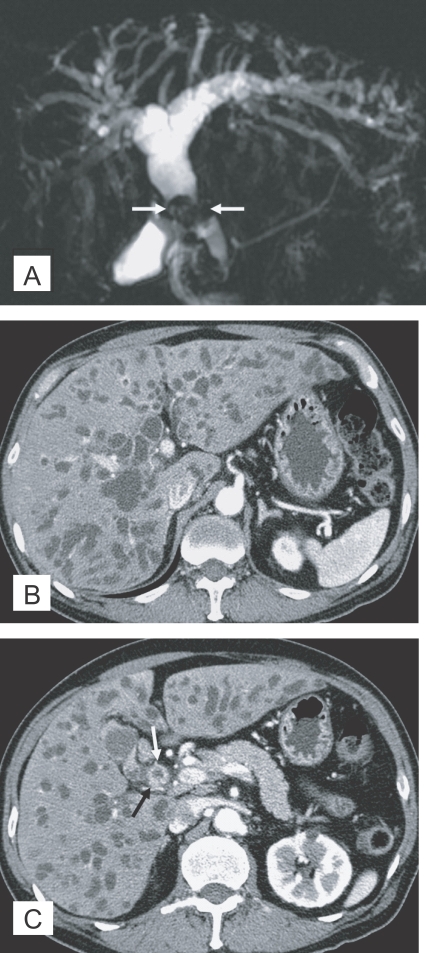
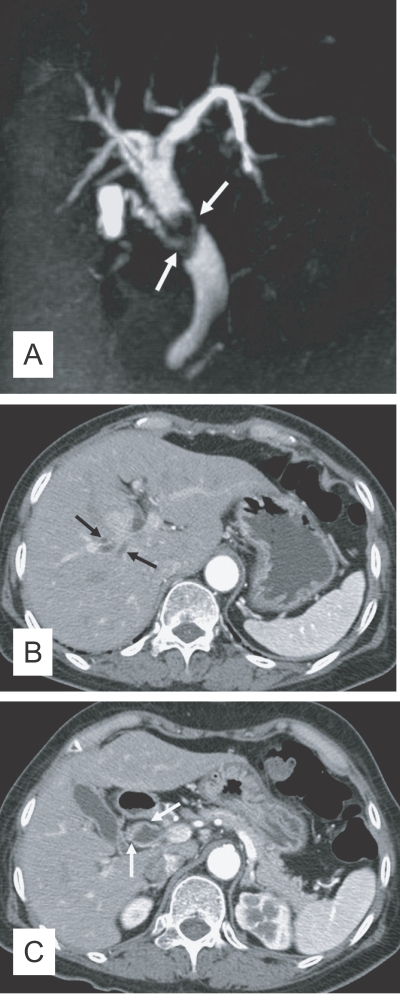
The imaging findings of clonorchiasis-associated cholangiocarcinomas are combinations of the findings of the 2 diseases (Figs. 5 and 6) (Choi et al., 2004). Diffuse dilatation of peripheral intrahepatic ducts is attributed to changes that are secondary to clonorchiasis, and segmental and severe dilatation around the tumor is caused by obstruction by the tumor (Fig. 5) (Choi et al., 1988 & 1989). Extrahepatic cholangiocarcinomas, associated with clonorchiasis, show diffuse dilatation of the peripheral and central intrahepatic bile ducts (Fig. 6). When an extrahepatic cholangiocarcinoma is not associated with clonorchiasis, dilatation of the peripheral intrahepatic bile ducts is not conspicuous (Fig. 7). After the development of the distal obstruction due to an extrahepatic cholangiocarcinoma, pre-existent dilated intrahepatic bile ducts with clonorchiasis easily progress the dilatation.
DIFFERENTIAL DIAGNOSIS OF CLONORCHIASIS
The differential diagnosis of clonorchiasis includes recurrent pyogenic cholangitis and primary sclerosing cholangitis. Recurrent pyogenic cholangitis is characterized by decreased branching and abrupt tapering of the peripheral hepatic ducts resulted from stenosis of the peripheral ducts (Lim, 1991; Kim et al., 1999). Dilatation of the extrahepatic bile duct and a stone on recurrent pyogenic cholangitis are more common than clonorchiasis. The pattern of intrahepatic bile duct dilation in clonorchiasis is diffuse, mild dilation of the intrahepatic bile duct without abrupt tapering of the peripheral hepatic ducts. However, because C. sinensis infection is one of the causes of recurrent pyogenic cholangitis, the mixed imaging findings of 2 disease entities are sometimes observed in a patient. Primary sclerosing cholangitis shows stenosis, beading and pruning of the dilated intrahepatic bile duct. However, the bile ducts in primary sclerosing cholangitis are much more irregular and serpiginous, which are unlikely in clonorchiasis (Ito et al., 1999). Of course, the primary sclerosing cholangitis is a very rare disease in endemic areas of clonorchiasis.
CONCLUSIONS AND PERSPECTIVES
Radiological examinations are essential in diagnosis of biliary tree diseases including clonorchiasis and cholangiocarcinomas. Clonorchiasis is primarily detected by screening sonography of the liver according to its pathognomonic findings of diffuse dilatation of the intrahepatic bile ducts, periductal echogenicity, and floating materials in the gallbladder. Periductal enhancement on dynamic contrast-enhanced CT or MR imaging may be a specific finding of active clonorchiasis. Imaging diagnosis is a good alternative method for diagnosis of clonorchiasis practically in endemic areas. Residents living in the endemic areas of clonorchiasis, who show images of diffuse dilatation of the intrahepatic bile ducts but have no history of specific medication, should be recommended to take praziquantel for treatment. For control of clonorchiasis in endemic areas, it is practically necessary to detect the infected residents by any diagnostic method, such as stool examination, serology, or radiological imaging.