A Case of Biliary Ascariasis in Korea
Article information
Abstract
Biliary ascariasis is still the leading cause of surgical complication of ascariasis, though its incidence has been dramatically reduced. Herein, we report a case of biliary ascariasis for the purpose of enhancing awareness of parasitic infections as a possible cause. A 72-year-old male visited the emergency room of Dankook University Hospital on 12 July 2015, complaining of right-upper-quadrant pain. By endoscopic retrograde cholangiopancreatography (ERCP), a tubular filling defect in the right hepatic duct was detected. The defect was endoscopically removed and diagnosed as an adult female of Ascaris lumbricoides worm, of 30 cm length. Upon removal of the worm, the pain subsided, and the patient was discharged without any complication. When treating cases of biliary colic, physicians should not neglect biliary ascariasis as the possible cause.
INTRODUCTION
Among the surgical complications of ascariasis, biliary migration of adult worms is the most common [1]. Although the natural habitat of Ascaris lumbricoides is usually in the jejunum, they can migrate to the biliary tract, causing biliary colic, obstructive jaundice, and cholelithiasis [2]. Between 1955 and 1989 in Korea, there were 1,198 reported cases of biliary ascariasis, which accounted for 92.2% of the overall surgical ascariasis patients [3]. Since that time, the incidences of ascariasis have been dramatically reduced; in fact, other than 2 cases in 2001 [4], there has been none reported. We report herein a case of biliary ascariasis for the purpose of enhancing awareness of parasitic infections as a possible cause.
CASE RECORD
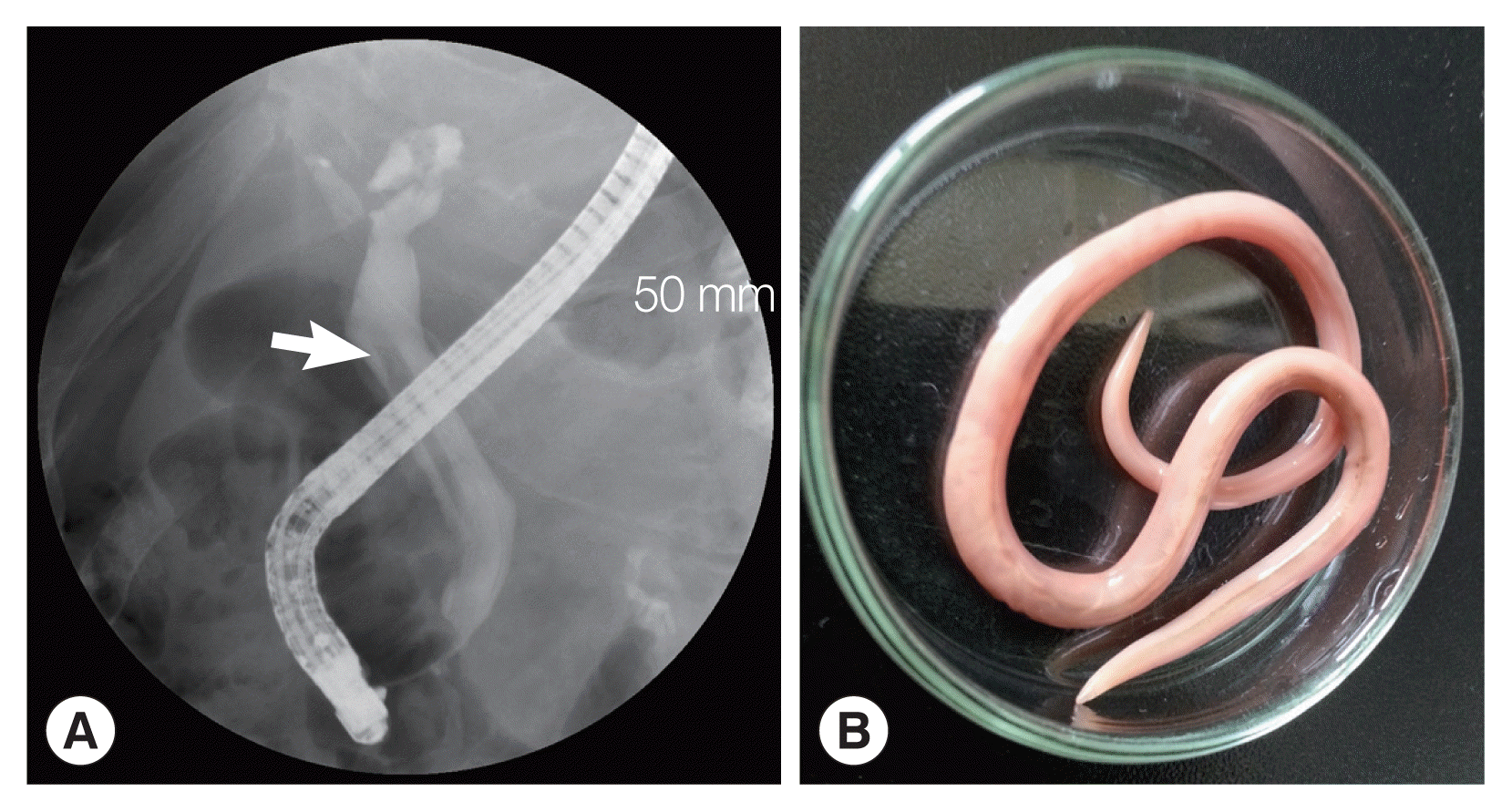
A 72-year-old male visited the emergency room of Dankook University Hospital on 12 July 2015, complaining of right upper quadrant pain. The pain began 15 days before the visit and had worsened by the day of admission. Interestingly, he had been suffering from recurrent hepatobiliary stones for a very long time, and should have undergone cholecystectomy and left hepatectomy 30 and 20 years before, respectively. Additionally, he had been treated for cholangitis due to a common bile duct (CBD) stone and sludge in 2014. On physical examination, no abnormal findings were observed, and the laboratory results were unremarkable except for mild elevation of as-partate aminotransferase, alanine aminotransferase, and gamma-glutamyl transferase (82 U/L, 114 U/L, 79 IU/L, respectively; normal range 0–40 U/L, 0–40 U/L, 8–61 IU/L, respectively). Total bilirubin and alkaline phosphatase were within normal limit (0.98 mg/dl and 86 IU/L, respectively; normal range 0.2–1 mg/dl, 40–129 IU/L). Cholangitis due to intrahepatic stone was suspected, and accordingly, the patient was referred for endoscopic retrograde cholangiopancreatography (ERCP). A tubular filling defect was detected in the right hepatic duct (Fig. 1A), and was proved to be a parasite by intraductal sonography. The parasite was endoscopically removed through the ampulla of Vater using the balloon sweeping method, and subsequently was diagnosed as an adult female of A. lumbricoides worm, of 30 cm length (Fig. 1B). After removal of the worm, the patient’s pain subsided. The patient thereupon was treated with albendazole, and discharged without any complication.
DISCUSSION
Although many hypotheses have been formed to explain the migration of A. lumbricoides to various organs, an important pre-requisite for their reaching the biliary tract seems to be a heavy infection [5]. In fact, these days, biliary ascariasis is seen more commonly in endemic countries [5]. In this respect, the recent discovery of biliary ascariasis in Korea seems exceptional. Therefore, even in Korea and other non-endemic countries, the possibility of ascariasis in cases of biliary colic should not be ruled out.
Another interesting finding in the current case was the repetitive formation of hepatobiliary stones. Although it has been suggested that hepatolithiasis can result from the presence of bacteria such as Klebsiella, Escherichia coli, and others, or from a carbohydrate-rich diet, parasitic infection should also be considered an important causative factor [6]. It is for this reason that, in East Asia, where A. lumbricoides and Clonorchis sinensis are prevalent, hepatolithiasis is endemic of 30–50% prevalence [7]. Notwithstanding, it would be hasty, of course, to assume an association between the frequent recurrence of hepatolithiasis in the patient and his parasitic infection.
In cases of suspicion of biliary ascariasis, ultrasonography (US) has been the imaging modality of choice; however, without careful examination, the diagnosis often is missed [8]. ERCP, alternatively, is a very useful tool, that effectively reveals the characteristic tubular filling defect within the biliary duct. Recently though, invasive ERCP has been replaced by magnetic resonance (MR) cholangiography as the preferred diagnostic procedure for biliary ascariasis [4]. By means of MR cholangiography repeated at 30 sec intervals, movement of live worms within the bile duct can be detected. This technique should be widely employed in the diagnosis of biliary diseases, especially parasite lodgment.
Although the rate of incidence of ascariasis has been dramatically reduced in Korea in recent decades, the estimated number of patients harboring A. lumbricoides was 15,754 in 2012; moreover, approximately 500,000 individuals from high-risk undeveloped countries have immigrated [9,10]. When physicians are presented with cases of biliary colic, therefore, biliary ascariasis should not be neglected as a possible cause.
ACKNOWLEDGMENT
This work was supported by a research fund of Dankook University in 2016.
Notes
CONFLICT OF INTEREST
We have no conflict of interest related to this work.