Intestinal protozoan infections and echinococcosis in the inhabitants of Dornod and Selenge, Mongolia (2003)
Article information
Abstract
The status of intestinal parasitic infections and seroprevalence of cystic echinococcosis in the inhabitants in Dornod and Selenge, Mongolia, was observed with stool and serum samples from 165 and 683 residents from August 9 to August 15, 2003. A total of 10 inhabitants (6.1%) were found to be infected with protozoan cysts or oocysts by stool examinations; 7, 1 and 2 cases with Entamoeba coli, Giardia lamblia and Cryptosporidium parvum, respectively. A total of 62 people (9.1%) revealed significantly high levels of specific antibodies against Echinococcus granulosus by enzyme-linked immunosorbent assay (ELISA). The surveyed areas are rural areas and the sanitized tab water is not available. There is a possibility of endemic transmission of water-borne protozoan diseases in these areas. The clinical echinococcosis is needed to be searched from the seropositive inhabitants.
The rate of human parasitic infection is affected by social, economic, climate, cultural and environmental factors. Most of parasites are distributed in tropical and subtropical areas in the world. Recently, some observations about parasite infections in Mongolia were reported, but the status is not well known. A little information on the seroprevalence of cystic echinococcosis (CE) is available. Survey for seroprevalence of CE by ELISA revealed that the positive rate ranged 5.2-8.5% in semi-nomadic pastoralists (Watson-Jones et al., 1997) or in the inhabitants near Ulaanbaatar (Lee et al., 1999). Studies were carried out between 1995 and 2000 in Bulgan, Mongolia. The prevalence of human hepatic CE by ultrasound was 0.2% (4/1,609) (Wang et al., 2005).
Twelve out of 67 dogs were reported to be Echinococcus egg positive (Zoljargal et al., 2001). Enterobiaisis is the most prevalent intestinal parasites due to their living pattern in ger, a Mongolian traditional housing pavilion. It was reported that 35.3% of schoolchildren in rural areas near Ulaanbaatar (138/391 cases) were Enterobius egg positive (Lee et al., 1999). Trichomoniasis, which is one of the most prevalent sexually transmitted protozoan diseases, is reported to be approximately 8 % (Garland et al., 2001).
In the present study, intestinal parasitic infections and echinococcosis in the inhabitants in a rural area of Mongolia were surveyed by stool examination and ELISA. A total of 165 stool and 683 serum samples were collected from August 9 to August 15, 2003, in Tsagaan ovoo Soum, Dornod Aymag and Orhon tuul Soum, Selenge Aymag, Mongolia. Dornod is the eastern area of Mongolia where examined inhabitants are mostly nomadic pastoralists. Selenge is the central and northern part of Mongolia where inhabitants are usually seminomadic pastoralists who also engaged in farming wheat (Fig. 1). Fifty stool samples were collected from Tsagaan ovoo Soum, Dornod, and the other 115 from Orhon tuul Soum, Selenge. In addition, 187 serum samples were collected from Tsagaan Ovoo Soum, Dornod, and 496 from Orhon tuul Soum, Selenge. Stools were examined by formalin-ethyl acetate concentration methods for helminth eggs and protozoan cysts and acid-fast stain for Cryptosporidium spp. For ELISA, micro-titer plates (Costar-Corning, Cambridge, California, USA) were coated with 200 µl of hydatid fluid (protein content: 2.5 µg/ml) in carbonate- bicarbonate buffer (pH 9.6) overnight at 4℃. Each serum was diluted at 1:100 in phosphate buffered saline containing 0.05% Tween 20 (PBS/T, pH 7.4), and incubated for 2 hr. Peroxidase conjugated anti-human IgG (Cappel, West Chester, Philadelphia, USA) was diluted at 1:1,000 and further incubated for 2 hr. The color reaction was developed by o-phenylenediamine, after which the reaction was stopped by adding 25 µl of 8 N H2SO4. Absorbance at 490 nm was recorded with a micro-titer plate reader (Bio-Rad M3550, Richmond, California, USA). Sera from normal controls, who denied any possible exposure to helminthic or protozoan parasites, were also tested. Cut-off absorbance for positive criterion was set at absorbance 0.25 after calibration employing sera from proven cystic echinococcosis, and mean + 3 SD of normal controls.
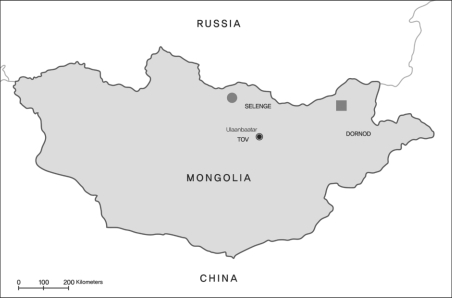
Surveyed areas: Tsagaan ovoo Soum in Dornod Aymag (▪) and Orhon tuul Soum in Selenge Aymag (●), Mongolia.
The results are summarized in Table 1. Out of 165 stools examined, we found 10 protozoan cyst or oocyst positive cases. They included 7, 1 and 2 cases of Entamoeba coli (4.2%), Giardia lamblia (0.6%) and Cryptosporidium parvum (1.2 %), respectively. There were no mixed infection cases. Helminth ova were not found in all stool samples examined. Of 7 E. coli-positive persons, 3 were males; the information on the sex of the 4 other inhabitants is unavailable. The cyst positive inhabitants were adults, but 2 children who were infected with C. parvum were 9 and 15 years old. Echinococcosis ELISA positive cases were detected in 62 (9.1 %) out of 683 sera. There were no mixed infections with intestinal parasitic infection and echinococcosis.

Results of stool examination and ELISA on the inhabitants of Dornod and Selenge in Mongolia, August 9-15, 2003
The present result demonstrated new information in the fauna of human parasites in Mongolia. Our results showed that C. parvum, E. coli and G. lamblia were found among Mongolian people. These protozoan infections mean that the contamination of the water or food with protozoa is present. In the surveyed areas, the tab water supply is limited and the well is the source of water for inhabitants. The absence of soil-transmitted helminthic infections is very interesting and it might be due to a small proportion of the farmer.
The seropositive rate of echinococcosis in Orhon tuul Soum was 11.7%, higher than those from previous reports (Watson-Jones et al., 1997; Zoljargal et al., 2001). The difference of seropositive rate of echinococcosis between Tsagaan ovoo Soum and Orhon tuul Soum might be attributed to the fact that the infection rate of E. granulosus in the definitive host, i.e., dog, showed some difference according to the province. The stool examination of the dogs in the surveyed area is needed to determine whether echinococcal infection of the dogs affects human echinococcosis. The seropositive echinococcosis inhabitants in Orhon tuul Soum is also needed to be followed by additional tests with ultrasonography and the chest radiography for the conformation of infection. Although the present result is localized information in a certain area of Mongolia, it shows that there would be a possibility of epidemics of water-borne protozoan infections in Orhon tuul Soum. The sanitation of the drinking water and foods should be monitored and the follow-up examination is required. Finally, more systematic approaches are needed to clarify the status of parasitic infections in Mongolia.
In Mongolia, test for enterobiasis in the primary schoolchildren have been screened regularly since more than 90% of the parasitic infections in the children is enterobiasis according to the enteric parasite laboratory of the National Research Center for Diseases, Mongolia (Ebright et al., 2003). The continuous surveillance system for monitoring the parasitic infection including enterobiasis in Mongolia is highly required to strengthen public health problems.
ACKNOWLEDGMENTS
We appreciate Dr. Yoon Kong, Department of Molecular Parasitology and Center for Molecular Medicine, Sungkyunkwan University School of Medicine and Samsung Biomedical Research Institute, Suwon, Korea, who kindly performed the serologic test for the sera of this work.
References
Notes
This study was supported by Grant M1-0306-03-0000 from the Ministry of Science & Technology, Republic of Korea.