Parasitic infections in HIV-infected patients who visited Seoul National University Hospital during the period 1995-2003
Article information
Abstract
The prevalence of parasitic infections was investigated in human immunodeficiency virus (HIV)-infected patients (n = 105) who visited Seoul National University Hospital, Seoul, Korea, during the period from 1995 to 2003. Fecal samples were collected from 67 patients for intestinal parasite examinations, and sputum or bronchoalveolar lavage samples from 60 patients for examination of Pneumocystis carinii. Both samples were obtained from 22 patients. Thirty-three (31.4%) of the 105 were found to have parasitic infections; Cryptosporidium parvum (10.5%; 7/67), Isospora belli (7.5%; 5/67), Clonorchis sinensis (3.0%; 2/67), Giardia lamblia (1.5%; 1/67), Gymnophalloides seoi (1.5%; 1/67), and Pneumocystis carinii (28.3%; 17/60). The hospital records of the 11 intestinal parasite-infected patients showed that all suffered from diarrhea. This study shows that parasitic infections are important clinical complications in HIV-infected patients in the Republic of Korea.
INTRODUCTION
Human immunodeficiency virus (HIV) infection is an extremely serious worldwide problem. As of 2004, about three thousand Koreans were reported to be infected with HIV by the National Institute of Health, Republic of Korea. Since the beginning of the HIV epidemic in the world, opportunistic infections have been recognized as an important clinical complication (Lebbad et al., 2001; Wiwanitkit, 2001; Vajpayee et al., 2003; Zali et al., 2004). In particular, opportunistic protozoans play a major role as etiologic agents of chronic diarrhea in HIV-infected patients. Chronic diarrhea in such patients can profoundly compromise the absorptive function of the small intestine, and cause significant mortality (Escobedo and Nunez, 1999). The protozoan parasites, Cryptosporidium parvum, Isospora belli, Cyclospora cayetanensis, Entamoeba histolytica, and Giardia lamblia are the causative agents of diarrhea among this population (Mohandas et al., 2003). In addition, Pneumocystis carinii pneumonia (PCP) remains the most common opportunistic infection associated with acquired immunodeficiency syndrome (AIDS) in developing countries (Wohl et al., 2002; Aderaye et al., 2003).
The detection of specific pathogens that cause severe diarrhea in HIV-infected patients has become a focus of interest, although such attempts have been limited, to date, in the Republic of Korea. Candidiasis and herpes virus infections were common gastrointestinal tract infections among the HIV-infected patients (Choi et al., 1999; Kim et al., 2003), however, no studies have focused specifically on opportunistic parasitic infections. Thus, the present study was undertaken to determine the prevalence of parasitic infections among HIV-infected patients in the Republic of Korea.
MATERIALS AND METHODS
Patients
One hundred and five HIV-infected patients who visited the Seoul National University Hospital, Seoul, Republic of Korea for check-up, and provided fecal, sputum, or bronchoalveolar lavage (BAL) samples, during the period from January 1995 to October 2003, were enrolled in this study. Fecal samples were obtained from 67 patients and sputum or BAL fluid from 60 (22 patients provided both sample types).
Examination of parasitic infections
Fecal samples were immediately fixed in 10% formalin, and processed using the formalin-ether sedimentation technique. The pellet obtained was smeared on a glass slide and observed under a light microscope. In addition, a second smear was made, air-dried, and stained using a modified acid-fast procedure to detect Cryptosporidium, Isospora, and other coccidian protozoa under a light microscope (× 1,000). Sputum was treated with 0.1 N KOH for 1 hr and washed with phosphate buffered saline. Sputum and BAL samples were centrifuged at 3,000 rpm for 10 min, smeared on a glass slides, and stained with Diff-Quik (Fisher Scientific, Orangeburg, NY, U.S.A.) to enable P. carinii infection diagnosis under a light microscope (× 1,000).
Review of medical records
The medical records of the 11 parasite-positive HIV-infected patients were reviewed; patients' experiences of diarrhea or fever were noted, as were the number of CD4+ cells at the time of the diagnosis of parasitic infections, weight loss, treatment, and effects of the treatment.
RESULTS
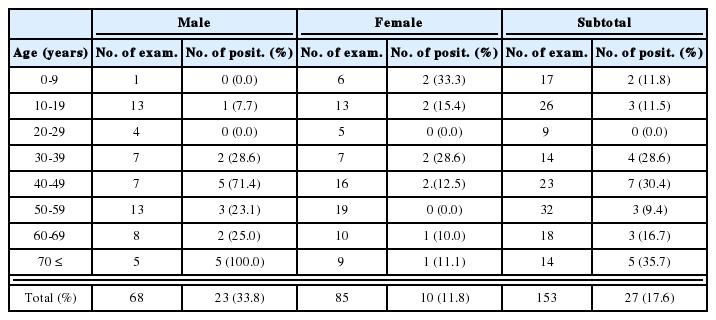
The mean age of patients who provided fecal samples was 39.2 ± 10.0 years (n = 67; 61 men and 6 women). Sixteen (23.9%) were found to be infected with intestinal (including liver) parasites (Table 1). Of these parasite-positive patients, the majority was men (80.0%) and more than 65% of the 16 were in their thirties and forties. Opportunistic protozoans predominated. The commonest was C. parvum (7/67; 10.5%) followed by I. belli (5/67; 7.5%) and G. lamblia (1/67; 1.5%). Helminthic infections were identified in 3 cases; Clonorchis sinensis (2/67; 3.0%) and Gymnophalloides seoi (1/67; 1.5%). Fifteen of these 16 positive cases were infected with one parasite species, and the single mixed case was infected with I. belli and G. seoi (Table 1).
The medical records of 11 parasite-infected patients showed that all or the majority experienced diarrhea (watery, bloody or non-specific) (11/11), weight loss (7/11), and fever (8/11) (Table 2). In 5 patients infected with C. parvum, the number of CD4+ lymphocytes was 50/mm3 or lower, whereas in 2 patients infected with I. belli, this number was 131/mm3 or higher. One of the two cases with the lowest CD4+ lymphocyte count of 10/mm3, was infected with G. lamblia; the other with C. sinensis. Three cases of cryptosporidiosis were treated with azithromycin, which provided a temporary effect in 2 cases and no effect in the other.
The mean age of patients subjected to a P. carinii examination was 38.9 years (n = 60), and 50 were men and 10 women. Of these 60 patients, 17 (28.3%) were infected with P. carinii (Table 1), with a mean age of 28.3 years and more than 80% were men. Most of them (12/17) suffered from respiratory difficulties or pneumonia.
DISCUSSION
Opportunistic infection continues to be a ubiquitous complication of advanced HIV infections and the one that exacts a heavy toll in terms of morbidity and mortality (Vajpayee et al., 2003). Despite recent increases in the number of HIV-infected patients in the Republic of Korea, few studies have been performed on the prevalence of opportunistic parasitic infections among those patients. In the present study, the prevalence of intestinal parasites and P. carinii infections among HIV-infected patients who visited Seoul National University Hospital during 1995 and 2003 was found to be high, i.e., 23.9% (16/67) and 28.3% (17/60), respectively. Overall parasite (including P. carinii) prevalence was 31.4% (33/105). With regard to intestinal parasites, no prior comparative report has been issued in the Republic of Korea, with the exception of two papers which focused on C. parvum and I. belli (Choi et al., 1999) or on Entamoeba histolytica (Oh et al., 2000). Oocysts of C. parvum or I. belli were detected in 3.5% (4/115) (Choi et al., 1999) and invasive amebiasis in 3.1% (6/195) of HIV-infected patients (Oh et al., 2000). With regard to PCP, our results were higher than the results previously reported in the Republic of Korea; 10.4% (18/173) (Oh et al., 1999) or 15.9% (28/176) (Kim et al., 2003) of HIV-infected patients.
Cryptosporidium parvum, an intracellular protozoan which parasitizes the intestinal mucosa and elicits transient diarrhea in healthy individuals, is also one of the most important opportunistic pathogens (Chai et al., 2001; Guk et al., 2003). In immunocompromised patients, this protozoan can cause severe and life-threatening diarrhea, which is often fatal (Chai et al., 2001). In the present study, most HIV-infected patients infected with C. parvum experienced severe watery diarrhea and weight loss. The prevalence of cryptosporidiosis is variable (> 0.5%-35% or higher) and depends on geography and the environment (Chai et al., 2001). Previous studies have indicated that CD4+ cells are important for host defense mechanisms against cryptosporidiosis (Guk et al., 2003). In 4 of 5 HIV-infected patients infected with C. parvum, CD4+ cell numbers were lower than in patients infected with I. belli. Moreover, no drug therapy has been shown to effectively treat cryptosporidiosis. It is of interest to note that 2 of 3 patients treated with azithromycin showed temporary effects.
Isospora belli had become more prominent in recent years because of its prevalence as an opportunistic pathogen in AIDS patients (Sorvillo et al., 1995). Nevertheless, no report is available on the prevalence of isosporiasis in the Republic of Korea. Moreover, the actual rate of this infection in immunocompetent individuals and HIV-infected patients is likely to be underestimated, because of the asymptomatic shedding of oocysts, treatment with trimethoprim-sulfamethoxazole (TMP-SMX) for other infections, a low number of oocysts excreted, and an inefficiency of feces concentration and oocyst observation (Escobedo and Nunez, 1999). Epidemiological studies on the prevalence of isosporiasis are required in the Republic of Korea.
Pneumocystis carinii, which is now more frequently classified as a fungus, is a ubiquitous organism that can cause interstitial pneumonia, and one of the common opportunistic parasites associated with AIDS in developing countries (Wohl et al., 2002). In the Republic of Korea, it was reported that 10.4% of 173 HIV-infected patients (Oh et al., 1999) and 15.9% of 176 patients (Kim et al., 2003) developed PCP. In our study, samples for the diagnosis of P. carinii infection were collected from HIV-infected and suspected to suffer from PCP. Most of them suffered from cough, dyspnea, sputum, and other respiratory symptoms. Therefore, a higher proportion (28.3%) was found to be infected in the present study. With regard to the treatment of PCP, primary prophylaxis with TMP-SMX was found to induce hypersensitivity in as many as 25% of HIV-infected patients (Fischl et al., 1988). However, no cases of hypersensitivity reactions to TMP-SMX have been reported in 46 Korean HIV-infected patients infected with P. carinii. The reason was suggested to be the fast speed of an acetylator status of Koreans (Oh et al., 1999). In the present study, we diagnosed P. carinii infection by Diff-Quik staining of sputum or BAL samples. Further studies are required to confirm the prevalence of this fungal infection using serology or other techniques.
The cause of death was checked in 11 HIV-infected patients, but we could find apparent causes of death in only 7 patients. Two HIV-infected patients infected with P. carinii died of sepsis and gastrointestinal bleeding, and three patients infected with C. parvum (one of the three was co-infected with P. carinii) died of pneumonia and liver abscess. Other patients infected with C. sinensis or I. belli died of pneumonia or disseminated tuberculosis.
The prevalence of helminthic infections in the present study was 4.5% (3/67) which included 2 clonorchiasis and 1 gymnophalloidiasis cases. These two species are important food-borne parasites in the Republic of Korea. In particular, G. seoi is transmitted by oysters, which are commonly eaten raw (Chai et al., 2003). This fluke parasitizes the small intestines of man and animals, and can induce gastrointestinal problems and varying degrees of indigestion (Chai et al., 2003).
The results of the present study demonstrate that opportunistic protozoan infections are prevalent among Korean HIV-infected patients and they represent an important source of clinical complications among these patients.
References
Notes
This study was supported by a grant from the Korea Science and Engineering Foundation [R05-2002-000-00808-0 (2002)] and by the BK21 Human Life Sciences project of the Ministry of Education, Republic of Korea.