INTRODUCTION
Sparganosis is an uncommon parasitic infection that is caused by tapeworms belonging to the genus Spirometra, specifically, its plerocercoid larva [1]. Sparganosis has been described from all over the world. However, case reports of patients are most prevalent in East Asia. Consuming undercooked snakes or frogs, drinking contaminated water, or coming to contact with infected skin by an open wound are just some of the ways that can begin the infection process [2]. It occurs usually in subcutaneous tissues of the patients, which then migrate to other tissues. Major symptoms of the patients with the sparganum include subcutaneous mass and obscure pain [3]. In humans, most common infection sites are abdominal wall and viscera, urogenital organs, extremities, central nervous system, chest, orbital region, neck, and oral cavity [4]. Cases of breast sparganosis is rare, representing less than 2% of all cases [5]. In most cases, the preoperative diagnosis of sparganosis is difficult, since it is a rare parasitic disease. Here, we report a case of surgically confirmed sparganosis from the right breast as well as its clinical, radiological, and pathological findings.
CASE RECORD
A 62-year-old woman came to our outpatient clinic, displaying a palpable right breast lump for 4–5 months. She experienced obscure discomfort in her right breast, without any nipple discharge or systemic symptoms. Recently, she experienced itching sensation of breast mass lesion as well. Physical examinations revealed a mobile and firm mass, within the normal overlying skin, without any palpable axillary lymph nodes. While she had often travelled to Southeast Asian countries, but she never ate snakes or frogs. However, while she was traveling, she could have taken impure water. Also, she was fond of raw beef, and she ate it regularly.
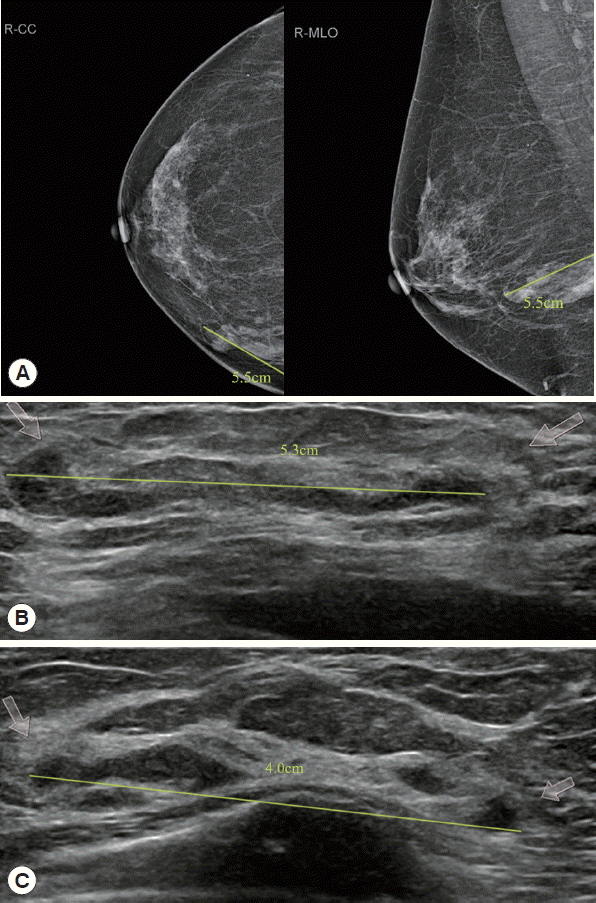
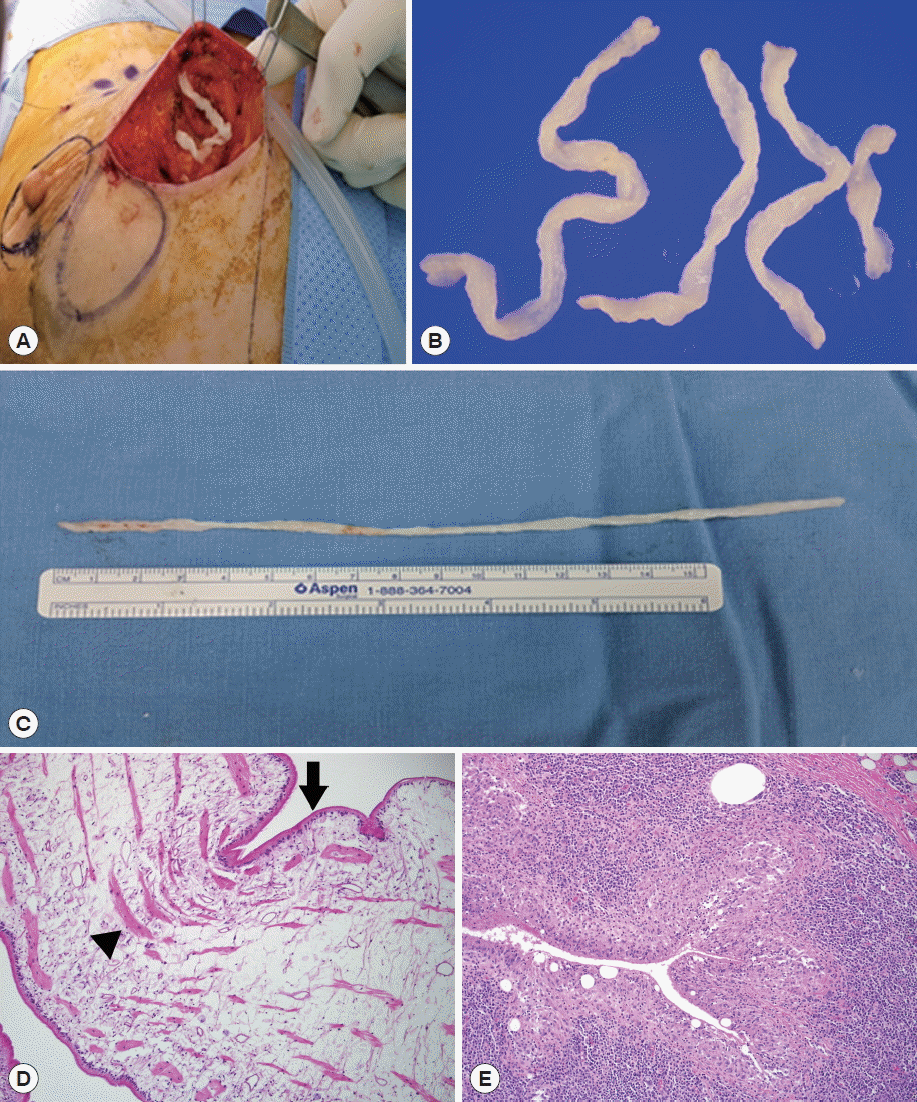
She visited a local clinic, and a core needle biopsy was performed. She came to our hospital. We suspected a parasitic infection and observed small fragments of worms on the histopathology slide. Mammography showed that the upper-inner quadrant of her right breast had a tubular lesion, about 5.5 cm in diameter. Breast ultrasonography also showed multiple track-like tubular lesions, about 5.3 cm diameter in the upper inner quadrant of her right breast and 4.0 cm diameter in the lower inner quadrant of her right breast (Fig. 1). The chest CT image demonstrated multiple, variable-sized, nodular, or tubular lesions in the medial aspect of the right breast, suggesting sparganosis. Abdominal, pelvic, and brain CT were taken and there were no significant abnormalities. During the operation, 4 pieces of a worm were visually identified (Fig. 2). The histopathologic findings revealed characteristic features of a sparganum and foreign body reaction in the excised breast parenchyme (Fig. 2). The patient’s symptoms were relieved after the removal of the breast mass. Anti-sparganum specific IgG level measured 1.22 by ELISA in patient’s serum. It was significantly higher than an uninfected control (0.22). However, the anti-sparganum specific IgG level was not examined after the operation.
DISCUSSION
Sparganosis is a parasitic infection caused by the plercercoid of the genus Spirometra. Sparganosis is more commonly found in the Far East, including China, Japan, and Korea [6]. Human infections occur from drinking water containing cyclops contaminated with procercoids or eating raw frogs and/or snakes. Our patient used water from a restaurant while she was traveling, and that was one instance when she could have taken impure water. The sparganum can migrate various tissues, including the subcutaneous tissues and muscles [2]. It can even migrate to the brain, abdominal wall, extremities, pleura, and bones; however, breast involvement is less than 2% of all cases [5].
In radiologic images, sparganosis most often appears as a nodular lesion. Therefore, it is difficult to distinguish it from soft tissues. Breast sparganosis presents with clinical symptoms that include palpable breast mass which may bring obscure pain, due to migration of the worm. However, peripheral blood eosinophilia and inflammatory reactions are rarely observed [7]. To rule out malignancy of the breast, a core needle biopsy is required in breast sparganosis. Our patient experienced a subcutaneous mass, vague pain, and itching sensation at the right breast. We found 4 pieces of a worm in the glandular mammary tissue of the right breast. The mammographic and ultrasonographic findings of breast sparganosis can be useful, for preoperative diagnosis and patient management [8]. Mammographic findings usually show a tapeworm-like structure; lobular or tubular lesion in the fat layer [8]. Ultrasonographic findings of sparganosis show several elongated tubular hypoechoic structures [2]. Pathology findings usually reveal foreign body reactions, including granulomatous inflammations along a track-like, elongated cavity, through which the sparganum passed [8]. In our patient, the removed sparganum was histologically characterized by eosinophilic tegument and longitudinal smooth muscle bundles in the loose internal stroma. Multiple cystic spaces in the breast parenchyme were surrounded by foreign body reactions with multinucleated giant cells and chronic inflammatory cells, such as plasma cells, lymphocytes, and a few eosinophils.
Surgical extraction is the confirmative diagnosis for sparganosis. For treatment of sparganosis, medication therapy, including praziquantel, is reported to have only limited effects [9]. Our patient was operated with complete surgical removal of breast masses with 4 pieces of a sparganum worm. Symptoms of the patient improved after the removal of the breast mass. Conclusively, we report a case of breast sparganosis that were confirmed by complete surgical excision. For the exact diagnosis, an inspection of mass site and detailed medical history and radiologic examination are important in preoperative diagnosis of sparganosis.